Post-Op Asymmetry
& Bridge Irregularity
Correction
A secondary rhinoplasty addressing post-operative nasal deviation, bridge irregularity, and tip imbalance following a primary procedure performed elsewhere two years prior.

Background &
Presenting Concerns
The patient, a 31-year-old woman, presented to the clinic 24 months following a primary open rhinoplasty performed by a different surgeon. Her initial procedure had aimed to reduce dorsal height and refine the nasal tip. While early results appeared satisfactory, she noticed progressive asymmetry and an irregular bridge contour as swelling resolved over the following year.
By the time of her consultation with Dr. Turan, she reported visible deviation of the nasal dorsum to the right, an irregular bridge with a visible step deformity at the rhinion, and a tip that appeared rotated and unprojected on the left side. She also noted intermittent nasal obstruction on the right, likely related to internal valve compromise from prior cartilage resection.
She had conducted extensive research and was seeking a surgeon with specific expertise in secondary procedures. Her primary goals were structural correction and a natural, balanced result — not a dramatically different appearance.
Case Overview
"I wasn't looking for a new nose — I just wanted the one I had planned when I first decided to have surgery."
Patient, Age 31
Before & After
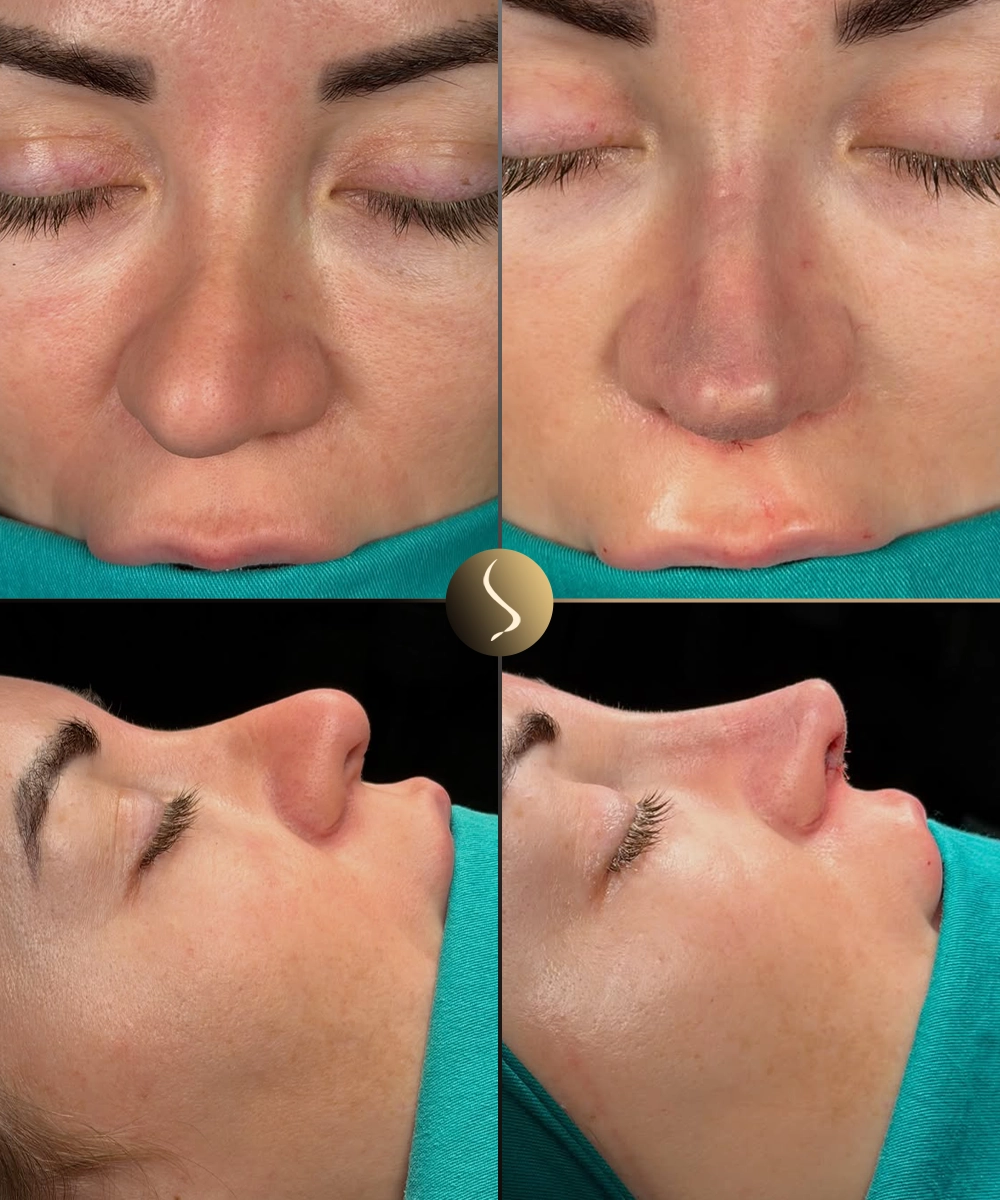
Photography taken on the same day under consistent lighting. Result shown at 12 months post-operative — when revision swelling is substantially resolved.
 Before
Frontal
Before
Frontal
 After
Frontal · 12 mo
After
Frontal · 12 mo
Frontal view: Note the correction of dorsal deviation and improved nasal symmetry from the midline. The bridge irregularity has been resolved and tip projection is balanced bilaterally. The skin envelope has fully re-draped over the reconstructed framework.
 Before
Profile (R)
Before
Profile (R)
 After
Profile (R) · 12 mo
After
Profile (R) · 12 mo
Right profile: The dorsal irregularity (step deformity at the rhinion) is resolved. A smooth, natural dorsal line has been achieved using a precise combination of cartilage grafting and rasping. Tip projection and rotation are restored to appropriate levels.
 Before
Oblique
Before
Oblique
 After
Oblique · 12 mo
After
Oblique · 12 mo
Oblique view: The three-quarter view confirms natural bridge contour, balanced tip definition, and harmonious nasal length proportions relative to the facial thirds. No visible irregularities, grafts, or asymmetry are apparent on the oblique assessment.
How the Revision
Was Approached
Every revision begins with understanding what was done before — identifying what structures are present, what was removed, and what must be rebuilt.
Pre-operative CT & Structural Analysis
A detailed CT scan was used to map the remaining septal cartilage, assess bone position, and identify the precise location and extent of the irregularity. Combined with physical examination under good lighting, this allowed a full picture of available reconstruction material before any incisions were planned.
Imaging · CT AnalysisOpen Approach via Original Columellar Incision
The prior columellar scar was excised and the nasal skin envelope carefully elevated. The degree of scar formation around the existing lower lateral cartilages was assessed intra-operatively. Existing cartilage grafts were identified and evaluated for stability and position.
Open Rhinoplasty · Scar RevisionDorsal Irregularity Correction
The step deformity at the rhinion was addressed with controlled rasping and placement of a precisely shaped spreader graft on the right side to re-establish dorsal symmetry. The asymmetric bony base was corrected with low-to-low osteotomies, bringing the nasal bones to a central position without over-mobilisation.
Spreader Graft · OsteotomyTip Reconstruction & Symmetry Restoration
The asymmetric lower lateral cartilages were repositioned and secured with dome-binding and inter-domal sutures. A small shield graft harvested from the concha was placed to improve tip definition and compensate for the under-projected side. Columellar strut reinforcement was added for long-term stability.
Shield Graft · Suture TechniquesInternal Valve Repair
Right-sided nasal obstruction was addressed with an alar batten graft placed at the internal valve angle. This technique expands the valve area without altering external appearance, and was the functional component of the procedure alongside the aesthetic correction.
Alar Batten Graft · FunctionalReconstruction Summary
Right spreader graftHarvested from residual septum · Dorsal symmetry
Low-to-low osteotomiesPercutaneous · Nasal base centralisation
Dome-binding suturesTip symmetry correction without grafts
Auricular shield graftConcha bowl harvest · Tip projection refinement
Columellar strutSeptal cartilage · Long-term tip support
Alar batten graft (R)Internal valve repair · Functional breathing
Rhinion raspingControlled reduction of step deformity
Moderately complex revision — multi-zone correction with structural graft requirement. Aesthetic + functional component.
Healing Milestones
Revision rhinoplasty heals more slowly than primary procedures due to scar tissue and altered blood supply. This timeline reflects this patient's documented recovery.
Immediate Recovery
Splint in place, elevation protocol, limited activity. Swelling and bruising peak at 48–72 hours then progressively reduce.
Splint Removal
External splint removed at day 10. Social presentability by week 3. Residual swelling remains, especially at the tip.
Early Healing
Tip softens, dorsal result becomes more apparent. Return to light exercise. Breathing improvement noticeable after nasal oedema reduces.
Major Milestone
Around 80% of final result visible. Tip definition improving. Dorsal correction fully stable. Photographed for interim documentation at this stage.
Final Documentation
Final photography session. Tip scar tissue fully matured. Graft integration complete. Result as shown in the gallery above.
12-Month Result
At 12 months, the patient demonstrates a natural, balanced nasal result with all presenting concerns addressed.
The bridge deviation and rhinion step have been corrected. The dorsal line is straight on both frontal and profile assessment.
Bilateral tip symmetry achieved. Projection is appropriate for facial proportions. No visible asymmetry on frontal, oblique, or worm's-eye views.
The patient reports significant improvement in right-sided nasal airflow. No further nasal obstruction symptoms at 12-month follow-up.
The result reads as a natural nose, not an operated one. Graft edges are imperceptible. Skin quality is preserved with no visible scarring beyond the columellar scar, which is well-healed.
"The success of this case depended entirely on the pre-operative plan. Once we understood exactly what had been done, the correction became a matter of precision rather than improvisation."
Dr. Selim Turan · Surgeon's Commentary


*All photographs are of this patient, taken at 12 months post-operative. Individual results vary.
Related Case Studies



Does This Case
Resemble Yours?
If you're dealing with similar concerns — asymmetry, bridge irregularity, or functional issues following a prior procedure — share the details with Dr. Turan's team. You'll receive an honest assessment of what's possible and what the revision process involves.
Share photos of your current nose (front, profile, oblique)
Describe your primary surgery — when, where, and what was done
List your main concerns — asymmetry, bridge, tip, breathing, or overall
Reference this case if your situation has similarities — it helps us understand your goals
🔒 Your details are confidential & never shared.